by: Kelly Witter, RN, MSN, CLC, CNE
Executive Summary
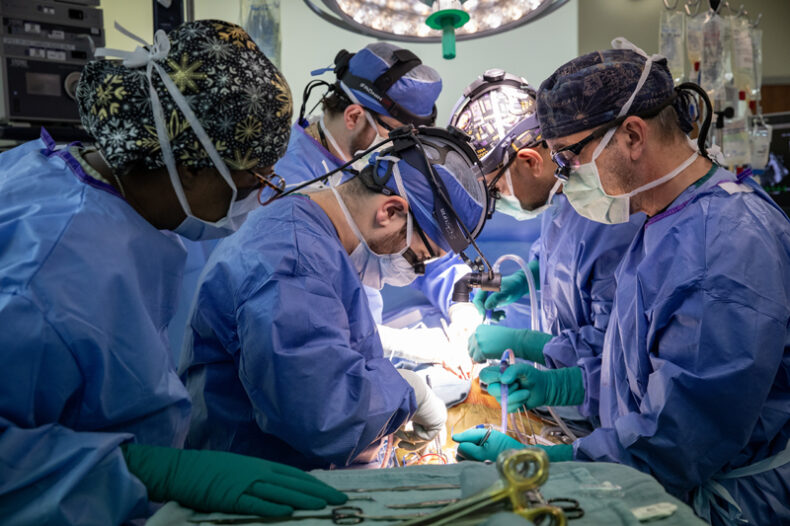
Transplant centers represent one of the most complex and mission-critical service lines within modern health systems. They operate at the convergence of advanced clinical care, multidisciplinary coordination, regulatory oversight, and significant financial exposure. As transplant demand continues to rise nationwide, programs are increasingly challenged to expand access, maintain outcomes, and ensure long-term sustainability amid workforce constraints and margin pressure.
National healthcare research consistently demonstrates that physician engagement, shared governance, operational discipline, and data transparency are essential to success in complex, high-acuity care environments. Yet many transplant programs continue to rely on operating models that separate clinical leadership from operational and strategic decision-making.
This white paper examines the structural challenges facing transplant centers, explores the characteristics of high-performing programs, and outlines an integrated, physician-aligned operating framework designed to support sustainable performance, innovation, and growth.
The Structural Complexity of Transplant Centers
Transplant programs differ fundamentally from most hospital service lines. Their complexity is driven not by a single factor, but by the interaction of multiple pressures:
- Scarce, highly specialized physician and clinical talent
- Multidisciplinary care models spanning inpatient, outpatient, and longitudinal follow-up
- Resource-intensive utilization of operating rooms, ICUs, and ancillary services
- Sensitivity to delays, variation, and downstream complications
- Heightened regulatory, accreditation, and quality expectations
- Ethical, emotional, and reputational considerations unique to transplant care
Despite this complexity, many transplant centers continue to operate within governance and operational structures designed for lower-acuity services. Research has shown that misalignment between clinical leadership and administrative oversight contributes to performance variability, inefficiency, and clinician dissatisfaction.³⁴
Why Traditional Management Models Fall Short
Historically, transplant centers have relied on one of two dominant management approaches:
- Clinically autonomous models, in which physicians retain decision-making authority but lack structured operational support, performance visibility, or accountability mechanisms.
- Administratively driven models, in which operational oversight exists but lacks clinical credibility or physician ownership.
Both approaches introduce risk. Clinically autonomous models may struggle with scalability, efficiency, and financial discipline. Administratively driven models frequently encounter resistance, disengagement, and cultural friction—particularly when decisions are perceived as disconnected from clinical realities.
Evidence across healthcare indicates that neither model is sufficient in isolation. Sustainable success requires integrated governance that aligns physicians and administrators around shared goals, supported by transparent data and disciplined execution.³⁴⁷
The Importance of Physician Alignment and Shared Governance
Physician alignment is not a compensation strategy or engagement tactic; it is an operating philosophy. In transplant centers, where clinical judgment and experience are central to care delivery, alignment must be embedded into governance and daily operations.
Effective physician-aligned governance structures:
- Integrate physician leaders into operational and strategic decision-making
- Establish shared accountability for quality, access, efficiency, and sustainability
- Clarify roles, authority, and escalation pathways
- Create a consistent cadence for performance review and action
Studies demonstrate that organizations with strong physician leadership and shared governance outperform peers in quality, operational efficiency, and financial performance, particularly in high-acuity service lines.
Operational Performance: From Variability to Predictability
Operational variability is one of the most significant threats to transplant center performance. Differences in workflows, scheduling practices, resource utilization, and care coordination can result in:
- Prolonged length of stay
- Capacity bottlenecks in ORs, ICUs, and clinics
- Delayed access for transplant candidates
- Increased staff strain and burnout
- Financial underperformance
High-performing transplant centers shift from reactive problem-solving to proactive operational management. This requires visibility into how care is delivered across the transplant continuum and the ability to identify bottlenecks before they affect outcomes.⁵⁶
Standardization in this context does not mean rigid clinical protocols. Instead, it involves creating predictable operational frameworks that support clinical excellence while reducing unnecessary variation.
Data as an Operational Asset, Not a Reporting Requirement
In many organizations, data is used primarily for retrospective reporting. In transplant programs, this approach is insufficient. High-performing centers treat data as an operational asset, a tool for decision-making, prioritization, and continuous improvement.
Actionable operational intelligence enables leaders to:
- Identify variation across providers, teams, and phases of care
- Understand capacity constraints and utilization patterns
- Track performance trends over time
- Support physician-led improvement initiatives with objective insight
When paired with aligned governance, data becomes a neutral and trusted foundation for collaboration rather than a source of conflict.¹⁷
Innovation in Transplant Center Operations
Innovation in transplant programs is often misunderstood as new technology or novel clinical techniques. While those elements matter, operational innovation is more fundamentally about how decisions are made and executed.
Leading transplant centers innovate by:
- Designing operating models that scale without increasing burnout
- Leveraging data to anticipate issues rather than react to them
- Embedding accountability into governance structures
- Aligning growth strategies with workforce sustainability
In this context, innovation is not disruptive, it is stabilizing. It brings clarity to environments historically characterized by complexity and variability.
How Dynafios Supports Transplant Centers
Dynafios partners with transplant centers to implement integrated performance models that align physicians, administrators, and operations around shared goals.
Unlike traditional consulting approaches, Dynafios emphasizes execution, sustainability, and physician credibility.
Physician-Aligned Governance
Dynafios works with transplant leadership to design governance structures that:
- Integrate physician leaders into operational oversight
- Clarify accountability and decision-making authority
- Support consistent, data-driven performance management
Operational Intelligence and Performance Visibility
Dynafios enables transplant centers to:
- Move beyond static reporting
- Identify operational drivers of variation and inefficiency
- Support proactive capacity and throughput management
Operational Optimization Across the Care Continuum
Dynafios supports improvement across:
- Pre-transplant evaluation and access
- Inpatient and procedural workflows
- Post-transplant coordination and follow-up
Technology-Enabled Execution
Dynafios technology is designed to:
- Enhance transparency and accountability
- Reduce administrative friction
- Enable consistent execution of governance decisions
- Scale alongside program growth
Strategic Growth and Sustainability
Dynafios helps transplant centers:
- Plan growth intentionally
- Align staffing and infrastructure with demand
- Protect physician engagement and long-term viability
Added Value and Differentiation
What differentiates Dynafios is an integrated approach that combines:
- Deep experience in physician-intensive service lines
- Credibility with both clinical and administrative leaders
- A focus on execution, not just strategy
- A long-term partnership mindset
This enables transplant centers to achieve meaningful improvement without compromising culture, mission, or clinical excellence.
Conclusion
Transplant centers face a future defined by increasing demand, constrained resources, and rising expectations. Success will not be achieved through incremental change or siloed management models.
By embracing physician-aligned governance, leveraging data as an operational asset, and innovating thoughtfully, transplant programs can improve performance while preserving the values that define transplant care. Dynafios stands as a strategic partner in this evolution.
Selected References
- Institute of Medicine. Best Care at Lower Cost: The Path to Continuously Learning Health Care in America. National Academies Press.
- McGlynn EA, et al. “The Quality of Health Care Delivered to Adults in the United States.” New England Journal of Medicine.
- Shortell SM, et al. “Physician Leadership and Hospital Performance.” Health Services Research.
- Bohmer RMJ. The Hard Work of Health Care Transformation. Harvard Business Review Press.
- United Network for Organ Sharing (UNOS). Transplant Trends, Outcomes, and Program Performance Metrics.
- Centers for Medicare & Medicaid Services. Hospital Quality and Performance Measurement Programs.
- Porter ME, Lee TH. “Why Strategy Matters Now.” New England Journal of Medicine.
- Healthcare Financial Management Association (HFMA). Optimizing Performance in Complex, High-Acuity Service Lines.
- Burns LR, Pauly MV. “Integrated Delivery Networks: A Detour on the Road to Integrated Health Care?” Health Affairs.